By Prof. Ricardo Lasmar (Brasil)
Uterine leiomyomas are frequent, have an impact on reproductive function and on women quality of life.
They are classified according to their location in the uterus, and submucosal fibroids would be most related to the uterine bleeding. When they are symptomatic, should be removed by surgery and the approach for myomectomy depends on their classification. In open and laparoscopic myomectomy after to incise the serosa and the myometrium, we start the blunt dissection in the plane between the myoma and its pseudocapsules. The uterine myoma pseudocapsule is a fibrous structure surrounding the neurovascular leiomyoma, separating it from the normal peripheral myometrium.
The fibroid pseudocapsule is composed of a rich neurovascular network in neurofibers similar to the neurovascular bundle surrounding the prostate.
In the larger fibroids, after being completely withdrawn from the uterine wall, they are morcellated. In no surgical technique of abdominal myomectomy the myoma is fragmented before removed from the uterine wall, it is always taken whole, mobilizing the nodule through the pseudocapsule. In this two surgical techniques, the myoma is fragmented after myomectomy, only to be retired of pelvis cavity.
In 1978, Neuwirth held the first hysteroscopic myomectomy using urological resectoscope with applying surgical technique similar to the resection of the prostate, with anresectoscope and “U” loop, slicing the fibroid and, sometimes, damaging the adjacent myometrium. The slicing technique fibroid, gold standard technique, leads to severe exposure lump vessels, causing greater blood loss, through strain absorption and sometimes myometrium damage with consequences for reproduction.
Some authors already make hysteroscopic myomectomy using the pseudocapsule. Litta et al, make the release after the resection of the intracavitary portion of the myoma, while Mazzon releases the intramural portion of the fibroid with cold loop. The technique published in Brazil in 2002 by our group uses the pseudocapsule in a similar form of the laparotomy or laparoscopic myomectomy, without partial resection of this, mobilizing the whole fibroid, believing that the integrity of pseudocapsule facilitates surgery.
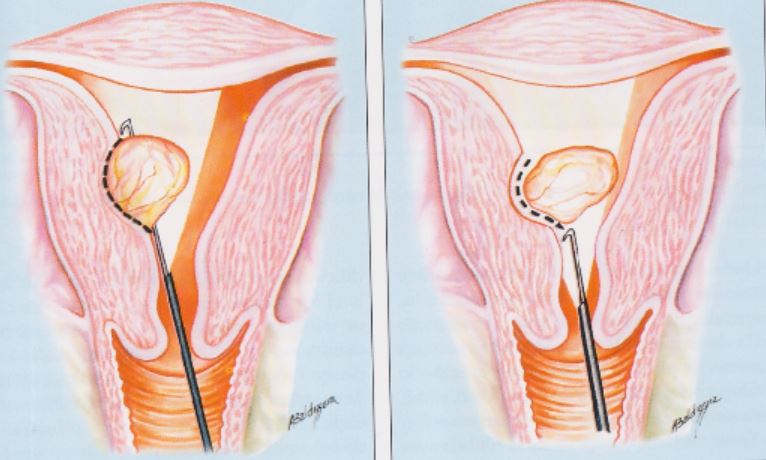
This technique, with the resectoscope with “L” loop (Collins), initiates with the incision of the myoma bed, surrounding it completely. From there, we enter the fibroid plan / pseudocapsule and releasing the fibrous bands, with occasional clotting of the vessels found. The vascular network generally surrounds the myoma, detachment of the myoma occurring inside the pseudocapsule should cause less bleeding and maintain the integrity myometrial, Allowing the facilitation of uterine healing and is of benefit for future reproductive outcome.
The first incision should always be done through the posterior portion, completely surrounding the endometrium until you reach the pseudocapsule. When reaching pseudocapsule starts the mobilizations of the nodule, with blunt dissection of the myoma pseudocapsule from adjacent myometrium, without cutting the nodule.
Only after the complete withdrawal of it we make sliced in the longitudinal direction and then, taken from the uterine cavity with grasping. In some larger fibroids, we make the myoma fragmentation before the complete liberation of the myometrium, because there is not enough space to mobilize the nodule in the uterine cavity.
The direct mobilization technique myoma prevents damage to adjacent myometrial and minimizes the risk of overload of the procedure. Moreover, during the mobilization of the fibroid, more intramural portion of the nodule is pushed by the myometrium to the uterine cavity, increasing the myometrium thickness and the distance of the fibroid to serosa, allowing the approach of fibroids with distances smaller than 5 mm to serosa safely.
The direct mobilization of the myoma is possible at the ambulatory surgery, doing the same movement with scissor around de pseudocapsule.
Hysteroscopy Newsletter